Part of Thermo Fisher Scientific
Material Safety Data Sheet
Organisms
Organisms this product works with:
PET-RPLA TOXIN DETECTION KIT
Code: TD0930
A kit for the detection of enterotoxin type A of Clostridium perfringens in faecal samples or culture filtrates by reversed passive latex agglutination.
INTRODUCTION
Food poisoning can result from eating foods contaminated with Clostridium
perfringens. The ingested cells multiply in the patients intestines and
produce spores. The production of enterotoxin is associated with this spore-forming
process. It is, therefore, important to detect the enterotoxin in faecal specimens
obtained from the patient or in the culture fluid of the bacterial isolates.
The direct detection of Cl.perfringens enterotoxins in faeces is the
most reliable method due to the much larger amount of toxin formed in vivo.
The culture method is less reliable due to problems in encouraging Cl. perfringens
to produce sufficient toxin in artificial media.
Reversed passive latex agglutination (RPLA) has been reported to be a reliable
method for the detection of Cl.perfringens enterotoxin.1 The
technique of reversed passive latex agglutination (RPLA) enables soluble antigen
such as bacterial toxins to be detected in an agglutination assay.
In a standard agglutination assay, soluble antibody reacts with particulate
antigen such as bacterial cells. However, in a reversed agglutination
assay the antibody, which is attached to particles, reacts with the soluble
antigen. The particles (in this case, latex) do not themselves play a part in
the reaction and they are therefore passive. The cross-linking of the
latex particles by the specific antigen/antibody reaction results in the visible
latex agglutination reaction.
PRINCIPLE OF ASSAY
Polystyrene latex particles are sensitised with purified antiserum taken
from rabbits immunised2 with purified Cl. perfringens enterotoxin.
These latex particles will agglutinate in the presence of Cl. perfringens
enterotoxin. A control reagent is provided which consists of latex particles
sensitised with non-immune rabbit globulins.
The test is performed in V-well microtitre plates. Dilutions of the culture
filtrate are made in two rows of wells, a volume of the latex suspension is
added to each well and the contents mixed. If Cl. perfringens enterotoxin
is present, agglutination occurs due to the formation of a lattice structure.
Upon settling, this forms a diffuse layer on the base of the well. If Cl.
perfringens enterotoxin is absent or at a concentration below the assay
detection level, no such lattice structure can be formed. A tight button will
therefore be observed.
PRECAUTIONS
This product is for in vitro diagnostic use only.
Do not freeze.
Reagents with different lot numbers should not be interchanged.
Reagents and diluent contain 0.1% sodium azide as a preservative. Sodium azide
may react with lead or copper plumbing to produce metal azides which are explosive
by contact detonation. To prevent azide accumulation in plumbing, flush with
copious amounts of water immediately after waste disposal.
STORAGE
The PET-RPLA Kit must be stored at 2-8°C. Under these conditions the reagents will retain their reactivity until the
date shown on the kit box. After reconstitution, the enterotoxin control should
be stored at 2-8°C. Under these conditions,
the reconstituted enterotoxin control will retain its reactivity for 3 months,
or until the date shown on the kit box, whichever is the sooner.
SAMPLE PREPARATION
The direct detection of Cl. perfringens enterotoxin in faeces is
the most reliable method and it should be followed unless insufficient faecal
materials is available. It is much quicker than the cultural method, taking
approximately 24 hours to obtain a result from sampling the faeces.
If the culture method is to be used for diagnosis of Cl. perfringens
food poisoning it should be noted that Cl. perfringens is a common inhabitant
of the bowel. It is recommended that at least 6 colonies are separately tested
to ensure a higher probability of detecting an enterotoxin-producing strain.
There is no single culture procedure which is suitable for all enterotoxin-producing
strains of Cl.perfringens. Any culture method used may fail due to insufficient
toxin production. This may be due to inadequate growth, poor spore formation
or low-level toxin production.
It should also be noted that some enterotoxin-positive strains may actually
be killed by heat treatment and will not, therefore, produce enterotoxin in
the second medium. It is recommended that each culture is checked for viability
after heating.
It is advisable to test the particular cultural method used with a known enterotoxin-producing
strain such as Cl. perfringens NCTC 8239 or Cl. perfringens ATCC®
12917.
METHOD OF USE
Materials required but not provided.
Microtitre plate (V-well) and lid.
Fixed or variable pipette and tips (25ml)
Centrifuge capable of generating 900g (typically 3000rpm in a small bench top
centrifuge) or membrane filtration unit using low protein-binding disposable
filters with a porosity of 0.2mm-0.45mm
(such as Millipore SLGV)
Culture media for proportion of enterotoxin production of Cl perfringens
strains (a suitable medium is that developed by Duncan and Strong3
modified by Harmon and Kautter1 (see Appendix)).
Sodium hypochlorite solution (>1.3%w/w)
25ml dropper (optional)
25ml diluter (optional)
Micromixer (optional)
Moisture box (optional)
Components of the Kit
Instruction Leaflet
TD931 Sensitised latex. Latex suspension sensitised with specific antibodies
(rabbit lgG) against Cl. perfringens enterotoxin.
TD932 Latex control. Latex suspension sensitised with non-immune rabbit
globulins.
TD933 Enterotoxin control Dried Cl. perfringens enterotoxin.
TD934 Diluent. Phosphate buffered saline containing bovine serum albumin.
Toxin Extraction or Production
Extraction from Faeces
To one volume of faeces, add a similar volume of phosphate buffered saline
(Oxoid BR14A).
Homogenise completely and centrifuge at 1300g for 20 minutes at 4°C then membrane filter using a 0.2mm - 0.45mm
low protein binding filter. The filtrate is then used as the test sample.
Production of Enterotoxin Culture Fluid
Culture the isolated organism in Cooked Meat Medium (Oxoid CM81) at 37°C for 18-20 hours, then inactivate by heating at 75°C for 20 minutes. Subculture to a medium designed for promotion of enterotoxin
production 3 4 .
Modified Duncan and Strong Medium 3,4
|
Formula |
gm/litre |
|
Yeast Extract (Oxoid L21) |
4.0 |
|
Proteose Peptone (Oxoid L85) |
15.0 |
|
Soluble starch |
4.0 |
|
Sodium thioglycollate |
1.0 |
|
NAsHPO47H20 |
10.0 |
Autoclave at 121°C for 15 minutes.
Add a sufficient amount of filter-sterilised 0.66M sodium carbonate to increase
the pH to 7.8 ± 0.1.
Inoculate 16 to 18ml of the medium with 0.8ml of the Cooked Mead Medium culture
(taken from the base of the tube). NOTE: If the dilution rate is greater
than 1:20, the Cooked Meat Medium constituents may be transferred in amounts
large enough to inhibit spore formation.
Incubate at 37°C for 24 hours. After incubation either centrifuge
at 900g for 20 minutes at 4°C and use the supernatant as the test sample
or membrane filter using a 0.2mm-0.45mm
low protein-binding filter and use the filtrate as the test sample.
Control
The reconstituted toxin control will agglutinate the sensitised latex. The
use of the toxin control will provide a reference for the positive patterns
illustrated below (see Interpretation of Test Results). The control should be
used from time to time only to confirm the correct working of the test latex.
The toxin control is not provided at a specified level and therefore must not
be used as a means of quantifying the level of toxin detected in the test sample.
Assay Method
Working Reagents
The latex reagents and diluent are ready for use. The latex reagents should
be thoroughly shaken before use to ensure a homogeneous suspension. To reconstitute
the enterotoxin control add 0.5ml of diluent (TD934) to each vial. Shake gently
until the contents are dissolved.
Arrange the plate so that each row consists of 8 wells. Each sample needs the
use of 2 such rows.
Using a pipette or dropper, dispense 25ml of diluent
in each well of the 2 rows except for the first well in each row.
Add 25ml of test sample to the first and second well
of each row.
Using a pipette or diluter and starting at the second well of each row,
pick up 25ml and perform doubling dilutions along
each of the 2 rows. Stop at the 7th well to leave the last well containing
diluent only.
Add 25ml of sensitised latex to each well of the
first row.
Add 25ml of latex control to each well of the second
row.
To mix the contents of each well, rotate the plate by micromixer or agitate
by hand. Take care that no spillage occurs from the wells.
To avoid evaporation, either cover the plate with a lid or place the plate in
a moisture box. Leave the plate undisturbed on a vibration-free surface
at room temperature for 20-24 hours. It will help subsequent reading of the
test if the plate is placed on black paper for the duration of this incubation.
Examine each well in each row for agglutination against a black background.
Centrifuge tubes, membrane filters, microtitre plates, lids and pipette tips
should be sterilised by autoclaving at 121°C or disinfected before disposal
in hypochlorite solutions (>1.3% w/w).
Dispose of toxin controls and culture extracts in hypochlorite solutions (>1.3%w/w).
INTERPRETATION OF RESULTS
The agglutination pattern should be judged by comparison with the following
illustration:
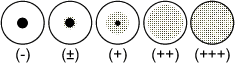
Results classified as (+), (++) and (+++) are considered to be positive.
In some cases, non-specific agglutination may be observed. If the faecal specimen
or culture filtrate reacts with the sensitised latex to a dilution greater than
that seen with the latex control, the test result should be regarded as positive.
The last well in all rows should be regarded as invalid.
LIMITATIONS OF THE TEST
The sensitivity of this test in detecting the enterotoxin is approximately
2ng/ml.
Enterotoxin present at concentrations lower than this will, therefore, give
negative results.
This kit is not intended for the detection of enterotoxins of other types of
Clostridium perfringens.
REFERENCES
1. Harmon, S M and Kautter, D A (1986). J. Food Prot. 49:
523.
2. Sakaguchi, G. Vemura, T. and Riemann, H.P. (1973). J Appl. Microbiol,
26: 762.
3. Duncan, C.L. and Strong, D H (1968). J. Appl. Microbiol.
1 : 82
4. Harmon, S.M. and Kautter, D.A. (1986). J. Food Protection 49:
706.
Copyright, Disclaimer and Privacy Policy | Conditions of Sale | About Us | Cookies
Thermo Fisher Scientific Inc.

